Outcomes of a Stress Management and Resiliency Training (SMART) Program for Family Caregivers of Individuals With Advanced Head and Neck Cancer
Objectives: To conduct a single-arm prospective pilot study examining the feasibility, acceptability, and preliminary effectiveness of a Stress Management and Resiliency Training (SMART) intervention among family caregivers (FCGs) of individuals with head and neck cancer (HNC).
Sample & Setting: This study was conducted with 26 FCGs of individuals with HNC receiving chemotherapy in the medical oncology clinic at the Mayo Clinic Comprehensive Cancer Center.
Methods & Variables: The SMART intervention consisted of in-person and online components. Measurements included feasibility, acceptability, self-compassion, resilience, perceived stress, anxiety, and mindfulness.
Results: Results support acceptability of the SMART program and provide recommendations to improve feasibility. Data indicate significant improvements in self-compassion (p = 0.03) and anxiety (p = 0.02), with positive trends for resilience, stress, and mindfulness.
Implications for Nursing: This study warrants further research with larger, more diverse samples testing the efficacy of the program, its mechanism of action, and potential synergistic effects among individuals receiving oncology care, FCGs, and nurses.
Jump to a section
According to the National Alliance for Caregiving (2021), an estimated 21% of adults in the United States are unpaid caregivers to an adult with health or functional needs, and 19% of these caregivers indicate that their own health is fair to poor. There are more than four million individuals who care for an adult with cancer in the home setting (AARP Family Caregiving, 2020), and a large majority of family caregivers (FCGs) report a high burden of care, negative emotions, and multiple unmet needs (National Cancer Institute, 2022). In 2021, there were 1,898,160 new cancer cases in America, with 66,630 being head and neck cancers (HNCs) (e.g., tongue, mouth, larynx, pharynx) (American Cancer Society, 2022). Treatment of HNC can involve surgery, radiation therapy, and chemotherapy, and it frequently consists of all three modalities (Schlichting et al., 2019). The burden of care for patients with HNC is great, and it often includes meticulous oral and skin care, tube feeding, tracheostomy care, hydration, enteral nutrition, and complex pain management (Paek et al., 2018).
FCGs are often thrust into their roles unexpectedly and experience a plethora of negative physical and emotional symptoms resulting from stress, which can lead to impaired sleep and immune function (Northouse, Williams, et al., 2012), greater risk for heart disease or musculoskeletal impairments (Kim et al., 2015), greater risk for some cancers (Shin et al., 2016), and long-term depression (Kim et al., 2014). FCGs can also experience poor health because of endocrine responses to stress, as well as exercise avoidance or smoking to cope with stress (Firth et al., 2020; Litzelman et al., 2018). FCGs can experience more distress than their care recipients and may have poorer overall psychological health, greater anxiety, and more fears of cancer recurrence. FCGs may also need to address alcohol and tobacco misuse in family members with HNC (Aupérin, 2020; Melin-Johansson et al., 2012; Williams & McCorkle, 2011). Stress is worse for FCGs when the patient is undergoing active cancer treatment or if the FCG is female or a spouse, has no choice in the caregiver role, spends more hours providing direct care, or experiences lifestyle modifications to provide tube feeding or tracheostomy care (Longacre et al., 2012). FCGs may provide care more than eight hours per day for up to two years for patients undergoing treatment (Given et al., 2012), and they often prioritize patient needs more than their own (Bevans & Sternberg, 2012).
Nurses have led research and practice initiatives to address caregiver needs for decades and know that when FCGs experience poor physical and emotional health, patient care suffers (Bevans & Sternberg, 2012; Given et al., 2012; Grady & Gullatte, 2014; Grady & Rosenbaum, 2015; Northouse, Katapodi, et al., 2012). When FCGs have unmet needs, there are negative influences on the patient’s physical health, mental health, and quality-of-life (QOL) outcomes (Douglas et al., 2016; Grady & Rosenbaum, 2015). Various types of interventions have been tested with FCGs of individuals with cancer, such as psychoeducation; skill development for coping, communication, and problem-solving; and counseling. However, reports of outcome variables from these interventions have been limited (Frambes et al., 2018). A review of studies assessing the outcomes of psychosocial care of FCGs of individuals with cancer identified that interventions could improve FCGs’ coping skills, knowledge, and QOL; however, these interventions are rarely implemented into practice (Northouse, Williams, et al., 2012).
Although negative outcomes of FCG stress are known, acknowledging the effect of potential protective factors, such as resilience, is an emerging concept (Peterson et al., 2014). Resilience can develop as a response to stress, but it can also lessen the negative effects of stress. Most oncology research has focused on resilience in patients only (Ghanei Gheshlagh et al., 2016; Hwang et al., 2018). However, in one study, a higher level of resilience in FCGs of patients with HNC was associated with less FCG distress (Simpson et al., 2015). In addition, identifying the benefits of caregiving has been found to contribute to positive outcomes for caregivers, such as improvement in the caregiver experience and the enhancement of overall caregiver well-being (Li & Loke, 2013).
Patients and families have consistently ranked compassionate care among their greatest healthcare needs (Sinclair et al., 2016). Compassionate care is particularly relevant to individuals with cancer and their caregivers because of the significantly higher intensity and burden of care required for individuals with cancer compared to other patients (National Alliance for Caregiving, 2016). Self-compassion (i.e., having compassion for oneself in a time of need) is a practice that has been consistently linked with reduced anxiety and depression, as well as improved emotional well-being, coping, and interpersonal relationships (Neff & Dahm, 2015). In addition, the cultivation of self-compassion has been associated with increased compassion for others (Neff & Pommier, 2013). Because depression and social isolation are two key risk factors for caregiver distress (Adelman et al., 2014), the practice of self-compassion among caregivers could mitigate burdens and lead to improved compassion and care for individuals with cancer.
Mindfulness interventions have been shown to reduce stress and anxiety for patients (Leppin et al., 2014) and FCGs (Li et al., 2016; Schellekens et al., 2017), as well as improve self-compassion in the general public (Birnie et al., 2010). However, one challenge for implementing mindfulness interventions among FCGs of individuals with cancer is that many programs necessitate six to eight sessions during a two-month period. Demands of caring for individuals receiving outpatient chemotherapy, particularly those with HNC, may prevent many FCGs from being able to engage in and finish these programs. This study examined the feasibility of and acceptability for FCGs of individuals with HNC undergoing outpatient chemotherapy to participate in a brief mindfulness intervention. This study is also a first step toward the goal of examining the influence of a brief mindfulness intervention on resilience, stress, anxiety, mindfulness, and self-compassion in FCGs of individuals with HNC.
During mindfulness practices, it is conceptualized there is simultaneous interplay among intention (why someone is practicing), attention (attending to the here and now), and attitude (nonjudgmental, with openness and compassion) (Shapiro et al., 2006). This interplay allows individuals to shift their perspectives from dwelling on the past or ruminating about the future to simply existing in the present moment and witnessing it without preconceptions (Brown et al., 2007; Shapiro et al., 2006). The Stress Management and Resiliency Training (SMART) program, developed by Amit Sood, MD, is a brief mindfulness program that guides participants to delay judgment and pay greater attention to the uniqueness of the environment around them rather than the contents of the mind. A key component of the program is the integration of mindfulness practices, such as attention training, to improve awareness of the present moment (Folkman & Greer, 2000; Lazarus, 1993) into everyday life to lessen stress (Sood et al., 2011; Sood & Jones, 2013).
The SMART program includes education on embracing the present moment with more gratitude, compassion, acceptance, and forgiveness, as well as refining interpretations of experiences by focusing on meaning and purpose. Through attention training, participants can experience increased relaxation as they engage in the present moment. This counteracts the default mode of excessive thinking about the past or the future, which leads to stress and anxiety (Brown & Ryan, 2003). Attention training is fostered through incorporating the following two mindful attention practices: joyful attention and kind attention. Joyful attention entails delaying judgment and paying attention to novelty, whereas kind attention entails sending silent, positive greetings to others (Sood et al., 2011). Finally, interpretation refinement is taught through practicing principles of gratitude, compassion, acceptance, meaning, forgiveness, celebration, reflection, and prayer (Sood & Jones, 2013).
The SMART program has been shown to provide improvements in resilience, anxiety, perceived stress, mindfulness, and QOL among breast cancer survivors (Loprinzi et al., 2011), physicians (Sood et al., 2011), radiologists (Sood et al., 2014), and nurses (Chesak et al., 2015, 2019, 2021; Magtibay et al., 2017). In a SMART/yoga study with caregivers and patients receiving transplantation, significant (p < 0.005) improvements were noted in perceived stress, depression, anxiety, and negative affect (Stonnington et al., 2016). Self-compassion outcomes of the SMART program have not yet been measured.
One key principle of the SMART program is compassion for self and others. Program content includes ways to practice compassion in daily life. The program is based on mindfulness principles, which are a key component of the practice of self-compassion (Germer & Neff, 2019). Self-compassion has been identified as an outcome of mindfulness-based practices (Golden et al., 2021). Implementing a SMART program intervention for FCGs has the potential to improve self-compassion, protect psychological health, and improve well-being. This, in turn, may support them in providing effective, compassionate care to patients.
There are many promising outcomes of mindfulness practices and resilience training programs, including the SMART program, in other populations. However, because of the paucity of studies with clear outcome variables for FCGs of individuals with cancer and the failure to implement studied interventions into practice, it is critical to test the feasibility, acceptability, and efficacy of interventions like the SMART program with FCGs and leverage outcomes to support future integration of mindfulness interventions for FCGs into practice. The purpose of this study was to examine the feasibility and acceptability of the SMART intervention when provided to FCGs of individuals receiving chemotherapy for advanced HNC. In addition, the investigators examined the preliminary effects of the SMART intervention on stress, self-compassion, resilience, anxiety, and mindfulness in FCGs.
Methods and Variables
Sample and Setting
This study was conducted with 26 FCGs, aged 18 years or older, of individuals with HNC who were receiving chemotherapy in the medical oncology clinic at the Mayo Clinic Comprehensive Cancer Center in Rochester, Minnesota. Inclusion criteria were (a) self-identifying as the primary caregiver of an individual with advanced HNC, (b) living with the care recipient at least 50% of the time, (c) having the ability to read and speak English, and (d) being cognitively intact. The exclusion criterion was having a severe mental health diagnosis, which would require a more supervised program.
A sample size of 20 is sufficient in pilot studies to meet the goals of feasibility of methods and acceptability to participants (Morris & Rosenbloom, 2017). Based on attrition rates in previous research with similar populations (Dose et al., 2017), target enrollment was increased to 26 to improve chances of having complete data on a total sample of 20 FCG participants.
This single-arm prospective pilot study was approved by the Mayo Clinic Institutional Review Board, and written consent as well as Health Insurance Portability and Accountability Act authorization was obtained by all study participants. The aims of the study were to (a) examine the feasibility and acceptability of the study procedures, measures, and intervention and (b) investigate the preliminary effectiveness of the SMART intervention on self-reported outcomes of self-compassion, resilience, perceived stress, anxiety, and mindfulness in FCGs at baseline and eight weeks after the initial intervention.
Recruitment
Participants were recruited from the medical oncology clinic at the Mayo Clinic Comprehensive Cancer Center. Potential participants were identified by clinicians and a study coordinator who conducted chart reviews to identify individuals whose FCGs would likely be eligible. FCGs of potential participants were approached by the study coordinator during the care recipient’s chemotherapy treatment appointment, and study inclusion and exclusion criteria were verified. Those who met the criteria were provided with information regarding the study protocols and were offered the opportunity to ask questions. If FCGs were undecided, they were provided with an informational flyer with study team contact information. Informed consent was obtained from those who agreed to participate.
Intervention
Following the consent process and the completion of baseline instruments, all participants attended a 90-minute small-group SMART session provided by study investigators. The SMART session consisted of education about stress responses and principles of compassion, gratitude, mindful presence, kindness, and a resilient mindset. Brief, practical exercises for gratitude and mindful presence of one to two minutes each were introduced and practiced. The format was interactive, informal, and adaptable to the group’s needs. After the group session, participants were instructed in using an online course with supplemental instructional videos for ongoing follow-up and skills practice during the eight-week study (Resilient Option, n.d.). Participants were also given a copy of the book The Mayo Clinic Guide to Stress-Free Living (Sood, 2013), which they were instructed to read during the eight-week study. The study team contacted participants by telephone every two weeks for the duration of the study to assess their progress and remind them to continue with the program components (see Figure 1). Samples of questions asked were as follows:
- Have you been able to practice the techniques offered during the small-group SMART session?
- If yes, about how many days have you practiced in the past two weeks?
- How much of the online course have you been able to complete in the past two weeks?
- How much of the book have you been able to complete in the past two weeks?

Measures
Feasibility was measured by numbers and percentages of participant recruitment, enrollment, and accrual; retention of participants in the SMART intervention study; and components of the SMART intervention used by participants. Other data related to participant recruitment, such as the number of potential eligible participants, the number excluded for each of the specific inclusion and exclusion criteria, and the number of participants who chose not to enroll, were also measured. Use of the intervention was measured by the number of days that study participants practiced the activities (SMART techniques, online course, book) related to the program, as well as by self-reported completion percentages.
Acceptability was measured by satisfaction with the research process using the Was It Worth It (WIWI) questionnaire (Chauhan et al., 2012). The WIWI questionnaire was developed to evaluate patient satisfaction with cancer clinical trial participation in the cooperative group setting, with results reported as individual items. No psychometric data for this tool are available. Acceptability and satisfaction with the SMART intervention were also measured using the program evaluation questionnaire developed by the investigators.
Effectiveness measures were conducted at baseline (prior to the small-group SMART session), and eight weeks later. These were self-report measures of perceived stress, self-compassion, resilience, anxiety, and mindfulness. Demographic data were also collected at baseline. The study team conducted measures by hand and entered them into a REDCap database (Harris et al., 2009).
Stress was measured using the Perceived Stress Scale (PSS) (Cohen et al., 1983), a 14-item, five-point Likert-type scale that provides a global measure of perceived stress in the past two weeks. Responses range from 0 (never) to 4 (very often), with higher scores indicating greater stress. The reliability of the PSS is adequate (alpha = 0.86), and it correlates with other instruments such as the Number of Life Events (r = 0.2, p < 0.01) and Impact of Life Events (r = 0.35, p < 0.01) (Cohen et al., 1983).
Self-compassion was measured using the Self-Compassion Scale–Short Form (SCS-SF), which provides a single global score for self-compassion (Raes et al., 2011). This 12-item, five-point scale with scores ranging from 1 (almost never) to 5 (almost always) measures compassion toward oneself in a time of need, with higher scores indicating greater self-compassion. The SCS-SF has demonstrated adequate internal consistency (alpha > 0.86) and correlates well with the long-form Self-Compassion Scale (r > 0.97).
Resilience was measured using the 10-item Connor-Davidson Resilience Scale (CD-RISC). Total scores range from 0 to 40, with higher scores indicating greater resilience. The CD-RISC has been found to have adequate internal consistency (alpha = 0.85), validity, and negative correlation with the PSS (r = –0.76, p < 0.001) (Campbell-Sills & Stein, 2007; Connor & Davidson, 2003).
Anxiety symptoms were measured using the Patient-Reported Outcomes Measurement Information System Short Form v1.0–Anxiety 8a (PROMIS Anxiety) (Cella et al., 2010). The PROMIS Anxiety answer options range from 1 (never) to 5 (always), with higher scores indicating greater anxiety. Its reliability has been reported as greater than 0.89, with strong correlation between the short form and the total item bank (r = 0.96) (Cella et al., 2010). Its correlations with other established instruments are strong, including the Center for Epidemiological Studies Depression Scale (r = 0.75) and the Mood and Anxiety Symptom Questionnaire (r = 0.8) (Cella et al., 2010).
Mindfulness was measured using the Mindfulness Attention Awareness Scale (MAAS), a 15-item, six-point Likert-type measure assessing mindfulness of moment-to-moment experiences. MAAS scores range from 1 (almost always) to 6 (almost never), with higher scores indicating greater mindfulness. The MAAS has adequate internal reliability (alpha = 0.89) (Brown & Ryan, 2003). Construct validity has been demonstrated through confirmatory factor analysis (Brown & Ryan, 2003; MacKillop & Anderson, 2007). Higher MAAS scores have been associated with lower mood disturbance as measured by the Profile of Mood States in individuals with cancer (r = –0.39) (Carlson & Brown, 2005).
Statistical Analysis
Data for participants who completed the study were entered into a REDCap database. Analyses were performed using SAS, version 9.4. Descriptive summaries were reported using mean and SD for age as a continuous variable and frequencies and percentages for categorical variables such as gender. Data collected from various scales (i.e., survey instruments) were summarized using median, minimum, and maximum because of non-normal distribution. There were 26 participants enrolled in this pilot study. Effectiveness of the SMART intervention was assessed using Wilcoxon signed-rank tests comparing measurements from baseline to week 8. Because of the pilot nature of the study and smaller sample size, no adjustments for multiple comparisons were performed. All tests were two-sided, and p values less than 0.05 were considered statistically significant.
Results
Demographics
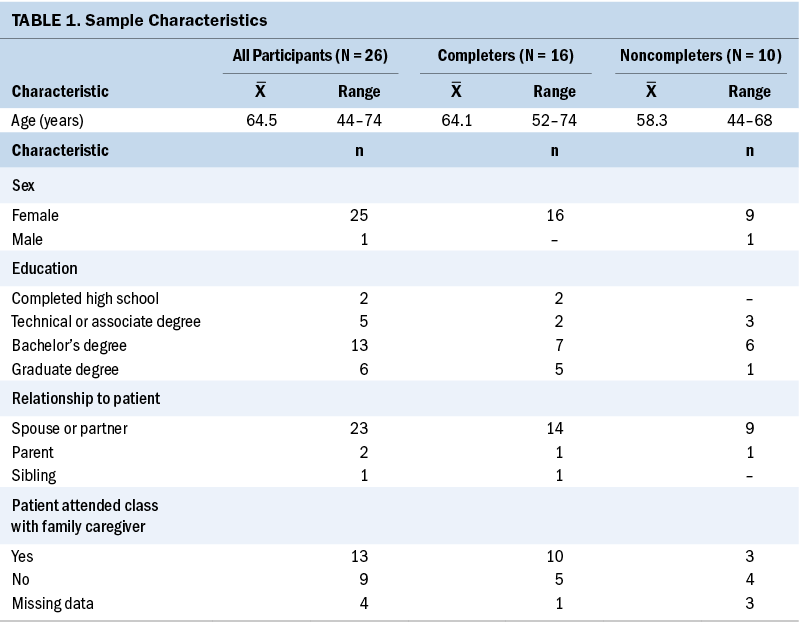
Twenty-six FCGs consented to participate, and 16 completed the study (defined as those who participated in the group session and completed measures at baseline and eight weeks). No participants dropped out of the study before the initial intervention. The participants were largely female (n = 25), had a mean age of 64.5 years, tended to hold a bachelor’s degree (n = 13), and were frequently the spouse or partner of the patient (n = 23). There was not a significant difference between the demographics of study completers and noncompleters (see Table 1).
Feasibility and Acceptability
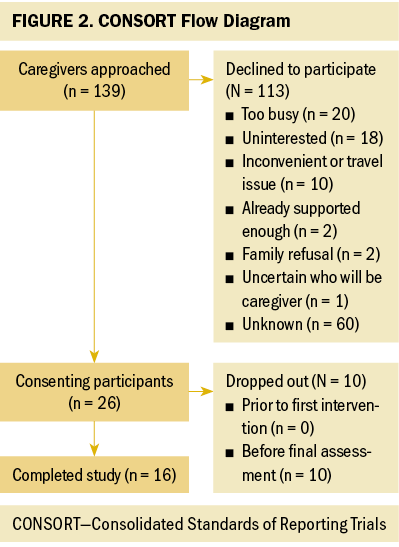
Of the 139 individuals who were approached to participate in the study, 26 agreed to participate (19% enrollment rate) and 16 completed the study (62% completion rate) (see Figure 2). No participants were excluded for inclusion or exclusion criteria. For those who did not agree to participate, 53 provided a reason such as too busy (n = 20), uninterested (n = 18), inconvenient or travel issue (n = 10), already supported enough (n = 2), family refusal (n = 2), and uncertain who will be the caregiver (n = 1).
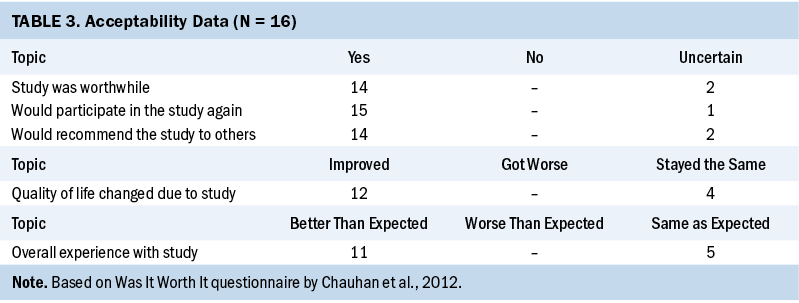
When study completers (n = 16) were asked how often they practiced the principles they learned in the small-group SMART session during the study period, most indicated they did so 41%–60% of the time (n = 7) (see Table 2). Responses to the WIWI questionnaire items showed that most study completers answered “yes” to the following: “Study was worthwhile” (n = 14), “would participate in the study again” (n = 15), and “would recommend the study to others” (n = 14). In addition, the majority indicated that their QOL had improved because of the study (n = 12), and their overall experience with the study was better than expected (n = 11) (see Table 3).
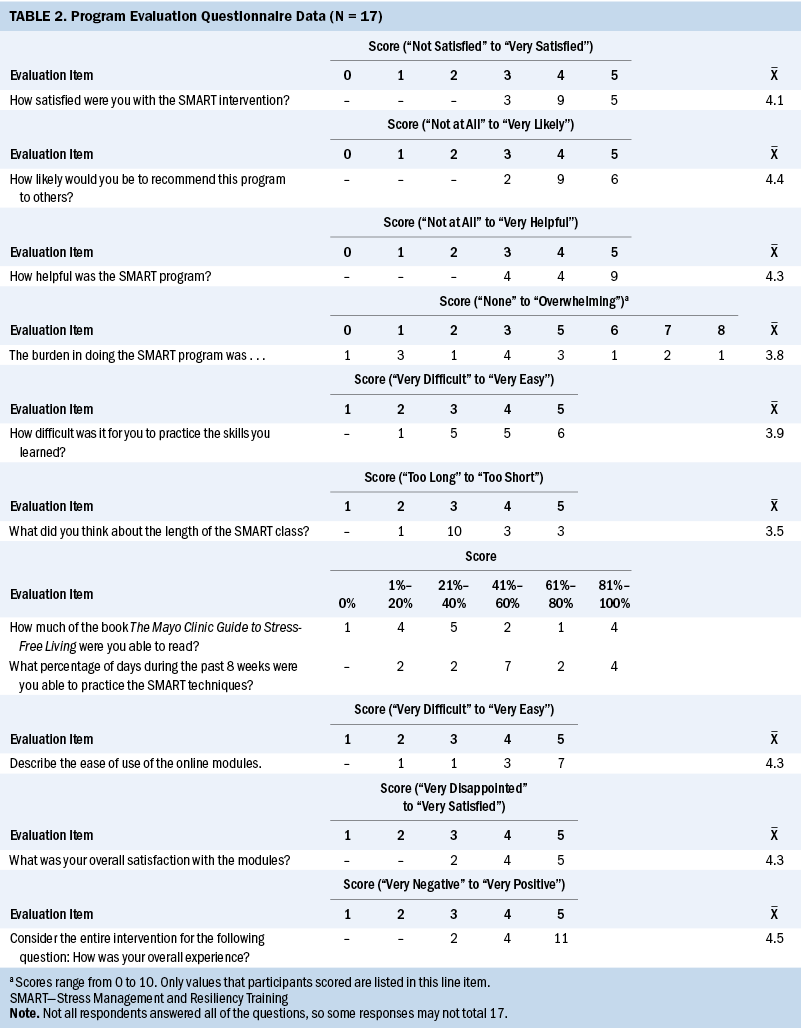
The program evaluation questionnaire was completed by 17 participants, and responses to the questions on the satisfaction portion of the questionnaire, measured on a scale from 1 (very disappointed, unlikely, or unhelpful) to 5 (very satisfied, likely, or helpful), indicated that most were either satisfied or very satisfied with the intervention (mean = 4.1), would likely recommend the program to others (mean = 4.4), and found the program helpful (mean = 4.3). When asked which aspects of the program participants liked the most, common themes were as follows: (a) the in-person class and the materials provided helpful information regarding understanding the brain and stress, such as how to override it with mindfulness, and having a choice about whether to be stressed; (b) the program provided stress management tools that were practical to begin immediately and fit into daily life; and (c) the online modules provided a convenient way to access the materials. One participant stated that “[the fact that] I was invited during a stressful situation [turned] my thinking around instantly after the class.” Another stated, “[The program] taught me a new way to focus—helped me to stay more in the moment—[to] be kind and make other people feel good.”
When asked what aspects of the program needed improvement, common themes were as follows: (a) would have been helpful to have the program before caregiving began; (b) would have liked a more effective way to follow up (suggestions included group follow-up meetings versus individual meetings and having some type of closure at the end of the program); (c) would have been helpful if the program was more tailored to caregivers; and (d) would have liked to have reminders to practice the principles of the program. One participant said that the individual follow-up calls did not provide much additional value, but it was “nice to have a compassionate voice on the other end.” Another stated, “I know I would get more out of this with discussion, hearing others’ thoughts.”
Effectiveness
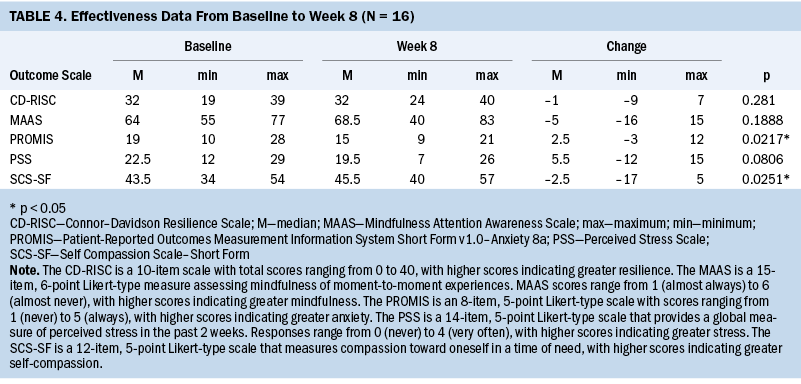
Five scales (PSS, SCS-SF, CD-RISC, PROMIS Anxiety, and MAAS) were used to assess the effectiveness of the SMART intervention. A descriptive summary of scores at baseline, week 8, and change from baseline to week 8, along with the p values from Wilcoxon signed-rank tests, is presented in Table 4. Statistically significant improvements in self-compassion (p = 0.0251) and anxiety (p = 0.0217) were observed among the 16 participants who provided data at both time points. Scores for stress (p = 0.806), resilience (p = 0.281), and mindfulness (p = 0.189) all improved from baseline to week 8, but improvements were not statistically significant.
Implications for Nursing
Findings from this pilot study show that the intervention was found to be acceptable among participants; however, additional work, such as optimizing recruitment and retention efforts, is needed to enhance feasibility. The recruitment and retention rates (19% and 62%, respectively) for this study were low compared to those identified in a review of literature regarding recruitment and retention in biobehavioral intervention studies with FCGs of individuals with cancer (Song et al., 2021). The literature review reported an average recruitment rate of 33% with a range of 8%–100%, and an average retention rate of 68% with a range of 19%–100% in the intervention arms across all studies (Song et al., 2021). Effective strategies to enhance recruitment in future studies are warranted, such as using relevant language for FCGs in recruitment materials (Hansen et al., 2017); recruiting purposefully through social media, at community outreach centers, and at events where FCGs of people with cancer would be (Hansen et al., 2017; Song et al., 2021); and streamlining the process of identifying and determining eligible participants who would be most likely to benefit from the intervention (Song et al., 2021). Effective strategies for retention, such as identifying the optimal time for enrollment within the course of the patient’s illness, designing interventions to be flexible, identifying the ideal length of the treatment time period and number of sessions, and reducing the number of follow-up assessments, are also warranted (Song et al., 2021). Finally, it would be beneficial to interview participants who dropped out of the study to identify their specific rationales.
Subsequent investigation of the acceptability, feasibility, and effectiveness of the SMART intervention would be beneficial in other groups of FCGs with high levels of distress, such as caregivers of patients with brain, spine, or nervous system cancers. Further research is also warranted to explore this program in a fully virtual capacity. The ability to participate virtually could address concerns about the COVID-19 pandemic as well as transportation or logistical challenges for busy FCGs, which may increase participation and satisfaction. Another study improvement could be to involve the patient in the intervention. Some evidence supports using dyadic interventions to improve stress and well-being in individuals with advanced lung cancer and their spouses (Milbury et al., 2020). Further research could also seek to identify which caregivers may benefit most from which types of supportive interventions, such as individual, dyadic, or group. Some participants provided feedback that they would appreciate a more effective way to follow up with the investigation team. A program could be developed to adapt to individual needs by providing more or fewer follow-up sessions for participants depending on their outcomes and preferences.
Caregivers for individuals with cancer receive psychosocial support from services such as social work or palliative care, but this often must be in conjunction with patient visits. There are few resources available that focus primarily on supporting caregivers. This intervention provides an opportunity for caregivers to come together and focus on their own self-care and resilience. Findings from the study demonstrate that participation in the SMART program led to significant improvements in self-compassion and anxiety for FCGs, as well as trends in a positive direction for stress, resilience, and mindfulness. Similar benefits were noted in a previous study with a SMART/yoga intervention for caregivers and patients receiving transplantation, where significant (p < 0.005) improvements were demonstrated in perceived stress, depression, anxiety, and negative affect (Stonnington et al., 2016). In addition, a SMART intervention with new nurses demonstrated positive trends in outcomes of stress, mindfulness, anxiety, and resilience (Chesak et al., 2015). In another study with nurse residents, significant (p < 0.001) improvements were noted for stress, mindfulness, and resilience in the intervention group compared to a control group (Chesak et al., 2021). In a study with experienced nurses, significant (p < 0.001) improvements were noted for stress, burnout, happiness, and mindful attention (Magtibay et al., 2017). Qualitative analysis from one of the studies found, among other outcomes, that the SMART intervention enhanced participants’ ability to manage emotionally taxing and task-oriented components of their roles, made them feel better about themselves, and increased their sense of calm (Chesak et al., 2019).
Outcomes from this study suggest that FCGs may experience similar benefits as professional caregivers from the SMART program. The findings indicating improved psychological health among FCG participants are supported by additional work from a systematic review across a population of caregivers, which shows that mindfulness-based programs can improve the psychological well-being of FCGs with various health conditions and diagnoses (Li et al., 2016).
Because study outcomes demonstrate support for the acceptability of the SMART program among FCGs, oncology nurses may want to participate in further SMART training with the goal of educating FCGs of patients with cancer. There should be future studies identifying whether nurses who integrate lessons from the SMART intervention and improve their own psychological well-being would be able to authentically educate patients and their FCGs using the program.
An evidence-based, easily accessible program to reduce stress and improve resilience, self-compassion, and mindfulness may help to improve psychological health and well-being among nurses faced with extensive job demands and complicated patient care requirements. Improving nurses’ well-being can benefit nurses directly and those they care for in an indirect or synergistic way.

Conclusion
The SMART program is acceptable among FCGs of individuals with advanced HNC, and efforts toward optimal feasibility (i.e., recruitment and retention strategies) are warranted for future studies. Effectiveness data demonstrated statistically significant improvements in self-compassion and anxiety, with positive trends for stress, resilience, and mindfulness. Limitations of the study were a small sample size, lack of control group, and lack of gender diversity among participants, as well as lack of race or ethnicity data. Additional research is warranted with larger numbers, a controlled design, and a more diverse sample to potentially enhance generalizability of results; identify which caregivers may benefit most from which types of supportive interventions, such as individual, dyadic, or group; determine the mechanism of action of the program; and identify whether nurses who care for individuals with complex healthcare needs would benefit in tandem with their care recipients in a synergistic way, from participating in the SMART program.

About the Authors
Sherry S. Chesak, PhD, RN, is a nurse scientist in the Division of Nursing Research, Ann Marie Dose, PhD, RN, is a principal health services analyst in the Division of Health Care Policy and Research in the Kern Center, and Jay Mandrekar, PhD, is a professor of biostatistics, all at the Mayo Clinic in Rochester, MN; Dara James, PhD, MS, is a postdoctoral scholar in the Edson College of Nursing and Health Innovation at Arizona State University in Phoenix; Deidre R. Pachman, MD, is a physician, Susanne Cutshall, DNP, APRN, CNS, is a clinical nurse specialist, and Debbie Lynn Fuehrer, MA, LPCC, is a mind–body medicine counselor and instructor in medicine, all at the Mayo Clinic; and Amit Sood, MD, is the executive director of the Global Center for Resiliency and Wellbeing in Rochester. This research was supported, in part, by an endowment to the Mayo Clinic Values Council from the Rochester Sisters of Saint Francis. Chesak, Dose, Cutshall, and Sood contributed to the conceptualization and design. Chesak, Cutshall, and Fuehrer completed the data collection. Mandrekar and James provided statistical support. Chesak, Mandrekar, James, Cutshall, Fuehrer, and Sood provided the analysis. All authors contributed to the manuscript preparation. Chesak can be reached at chesak.sherry@mayo.edu, with copy to ONFEditor@ons.org. (Submitted January 2022. Accepted May 19, 2022.)
References
AARP Family Caregiving. (2020). Caregiving in the U.S. https://www.caregiving.org/wp-content/uploads/2021/01/full-report-careg…
Adelman, R.D., Tmanova, L.L., Delgado, D., Dion, S., & Lachs, M.S. (2014). Caregiver burden: A clinical review. JAMA, 311(10), 1052–1060. https://doi.org/10.1001/jama.2014.304
American Cancer Society. (2022). Estimated number of new cancer cases and deaths by state—2021. https://www.cancer.org/content/dam/cancer-org/research/cancer-facts-and…
Aupérin, A. (2020). Epidemiology of head and neck cancers: An update. Current Opinion in Oncology, 32(3), 178–186. https://doi.org/10.1097/CCO.0000000000000629
Bevans, M., & Sternberg, E.M. (2012). Caregiving burden, stress, and health effects among family caregivers of adult cancer patients. JAMA, 307(4), 398–403. https://doi.org/10.1001/jama.2012.29
Birnie, K., Speca, M., & Carlson, L.E. (2010). Exploring self-compassion and empathy in the context of mindfulness-based stress reduction (MBSR). Stress and Health, 26(5), 359–371. https://doi.org/10.1002/smi.1305
Brown, K.W., & Ryan, R.M. (2003). The benefits of being present: Mindfulness and its role in psychological well-being. Journal of Personality and Social Psychology, 84(4), 822–848. https://doi.org/10.1037/0022-3514.84.4.822
Brown, K.W., Ryan, R.M., & Creswell, J.D. (2007). Mindfulness: Theoretical foundations and evidence for its salutary effects. Psychological Inquiry, 18(4), 211–237. https://doi.org/10.1080/10478400701598298
Campbell-Sills, L., & Stein, M.B. (2007). Psychometric analysis and refinement of the Connor–Davidson Resilience Scale (CD-RISC): Validation of a 10-item measure of resilience. Journal of Traumatic Stress, 20(6), 1019–1028. https://doi.org/10.1002/jts.20271
Carlson, L.E., & Brown, K.W. (2005). Validation of the Mindful Attention Awareness Scale in a cancer population. Journal of Psychosomatic Research, 58(1), 29–33. https://doi.org/10.1016/j.jpsychores.2004.04.366
Cella, D., Riley, W., Stone, A., Rothrock, N., Reeve, B., Yount, S., . . . Hays, R. (2010). The Patient-Reported Outcomes Measurement Information System (PROMIS) developed and tested its first wave of adult self-reported health outcome item banks: 2005–2008. Journal of Clinical Epidemiology, 63(11), 1179–1194. https://doi.org/10.1016/j.jclinepi.2010.04.011
Chauhan, C., Atherton, P.J., Satele, D., Dueck, A.C., Soori, G.S., Johnson, D.B., . . . Sloan, J.A. (2012). Patient satisfaction with participation in phase II/III NCCTG clinical trials: Was it worth it? (N0392). Journal of Clinical Oncology, 30(15, Suppl.), 6133. https://doi.org/10.1200/jco.2012.30.15_suppl.6133
Chesak, S.S., Bhagra, A., Schroeder, D.R., Foy, D.A., Cutshall, S.M., & Sood, A. (2015). Enhancing resilience among new nurses: Feasibility and efficacy of a pilot intervention. Ochsner, 15(1), 38–44.
Chesak, S.S., Morin, K.H., Cutshall, S.M., Carlson, M., Joswiak, M.E., Ridgeway, J.L., . . . Sood, A. (2019). Stress Management and Resiliency Training in a nurse residency program: Findings from participant focus groups. Journal for Nurses in Professional Development, 35(6), 337–343. https://doi.org/10.1097/NND.0000000000000589
Chesak, S.S., Morin, K.H., Cutshall, S.M., Jenkins, S.M., & Sood, A. (2021). Feasibility and efficacy of integrating resiliency training into a pilot nurse residency program. Nurse Education in Practice, 50, 102959. https://doi.org/10.1016/j.nepr.2020.102959
Cohen, S., Kamarck, T., & Mermelstein, R. (1983). A global measure of perceived stress. Journal of Health and Social Behavior, 24(4), 385–396. https://doi.org/10.2307/2136404
Connor, K.M., & Davidson, J.R.T. (2003). Development of a new resilience scale: The Connor–Davidson Resilience Scale (CD-RISC). Depression and Anxiety, 18(2), 76–82. https://doi.org/10.1002/da.10113
Dose, A.M., Hubbard, J.M., Mansfield, A.S., McCabe, P.J., Krecke, C.A., & Sloan, J.A. (2017). Feasibility and acceptability of a dignity therapy/life plan intervention for patients with advanced cancer. Oncology Nursing Forum, 44(5), E194–E202. https://doi.org/10.1188/17.ONF.E194-E202
Douglas, S.L., Daly, B.J., & Lipson, A.R. (2016). Relationship between physical and psychological status of cancer patients and caregivers. Western Journal of Nursing Research, 38(7), 858–873. https://doi.org/10.1177/0193945916632531
Firth, J., Solmi, M., Wootton, R.E., Vancampfort, D., Schuch, F. B., Hoare, E., . . . Stubbs, B. (2020). A meta-review of “lifestyle psychiatry”: The role of exercise, smoking, diet and sleep in the prevention and treatment of mental disorders. World Psychiatry, 19(3), 360–380. https://doi.org/10.1002/wps.20773
Folkman, S., & Greer, S. (2000). Promoting psychological well-being in the face of serious illness: When theory, research and practice inform each other. Psycho-Oncology, 9(1), 11–19.
Frambes, D., Given, B., Lehto, R., Sikorskii, A., & Wyatt, G. (2018). Informal caregivers of cancer patients: Review of interventions, care activities, and outcomes. Western Journal of Nursing Research, 40(7), 1069–1097. https://doi.org/10.1177/0193945917699364
Germer, C., & Neff, K. (2019). Teaching the mindful self-compassion program: A guide for professionals. Guilford.
Ghanei Gheshlagh, R., Sayehmiri, K., Ebadi, A., Dalvandi, A., Dalvand, S., & Nourozi Tabrizi, K. (2016). Resilience of patients with chronic physical diseases: A systematic review and meta-analysis. Iranian Red Crescent Medical Journal, 18(7), e38562. https://doi.org/10.5812/ircmj.38562
Given, B.A., Given, C.W., & Sherwood, P. (2012). The challenge of quality cancer care for family caregivers. Seminars in Oncology Nursing, 28(4), 205–212. https://doi.org/10.1016/j.soncn.2012.09.002
Golden, H.L., Vosper, J., Kingston, J., & Ellett, L. (2021). The impact of mindfulness-based programmes on self-compassion in nonclinical populations: A systematic review and meta-analysis. Mindfulness, 12(1), 29–52. https://doi.org/10.1007/s12671-020-01501-8
Grady, P.A., & Gullatte, M. (2014). The 2014 National Nursing Research Roundtable: The science of caregiving. Nursing Outlook, 62(5), 362–365. https://doi.org/10.1016/j.outlook.2014.05.007
Grady, P.A., & Rosenbaum, L.M. (2015). The science of caregiver health. Journal of Nursing Scholarship, 47(3), 197–199. https://doi.org/10.1111/jnu.12137
Hansen, D., Sheehan, D.K., & Stephenson, P. (2017). Family caregiver recruitment via social media: Challenges, opportunities and lessons. International Journal of Palliative Nursing, 23(2), 84–87. https://doi.org/10.12968/ijpn.2017.23.2.84
Harris, P.A., Taylor, R., Thielke, R., Payne, J., Gonzalez, N., & Conde, J.G. (2009). Research electronic data capture (REDCap)—A metadata-driven methodology and workflow process for providing translational research informatics support. Journal of Biomedical Informatics, 42(2), 377–381. https://doi.org/10.1016/j.jbi.2008.08.010
Hwang, I.C., Kim, Y.S., Lee, Y.J., Choi, Y.S., Hwang, S.W., Kim, H.M., & Koh, S.-J. (2018). Factors associated with caregivers’ resilience in a terminal cancer care setting. American Journal of Hospice and Palliative Medicine, 35(4), 677–683. https://doi.org/10.1177/1049909117741110
Kim, Y., Carver, C.S., Shaffer, K.M., Gansler, T., & Cannady, R.S. (2015). Cancer caregiving predicts physical impairments: Roles of earlier caregiving stress and being a spousal caregiver. Cancer, 121(2), 302–310. https://doi.org/10.1002/cncr.29040
Kim, Y., Shaffer, K.M., Carver, C.S., & Cannady, R.S. (2014). Prevalence and predictors of depressive symptoms among cancer caregivers 5 years after the relative’s cancer diagnosis. Journal of Consulting and Clinical Psychology, 82(1), 1–8. https://doi.org/10.1037/a0035116
Lazarus, R.S. (1993). Coping theory and research: Past, present, and future. Psychosomatic Medicine, 55(3), 234–247. https://doi.org/10.1097/00006842-199305000-00002
Leppin, A.L., Bora, P.R., Tilburt, J.C., Gionfriddo, M.R., Zeballos-Palacios, C., Dulohery, M.M., . . . Montori, V.M. (2014). The efficacy of resiliency training programs: A systematic review and meta-analysis of randomized trials. PLOS ONE, 9(10), e111420. https://doi.org/10.1371/journal.pone.0111420
Li, G., Yuan, H., & Zhang, W. (2016). The effects of mindfulness-based stress reduction for family caregivers: Systematic review. Archives of Psychiatric Nursing, 30(2), 292–299. https://doi.org/10.1016/j.apnu.2015.08.014
Li, Q., & Loke, A.Y. (2013). The positive aspects of caregiving for cancer patients: A critical review of the literature and directions for future research. Psycho-Oncology, 22(11), 2399–2407. https://doi.org/10.1002/pon.3311
Litzelman, K., Kent, E.E., & Rowland, J.H. (2018). Interrelationships between health behaviors and coping strategies among informal caregivers of cancer survivors. Health Education and Behavior, 45(1), 90–100. https://doi.org/10.1177/1090198117705164
Longacre, M.L., Ridge, J.A., Burtness, B.A., Galloway, T.J., & Fang, C.Y. (2012). Psychological functioning of caregivers for head and neck cancer patients. Oral Oncology, 48(1), 18–25. https://doi.org/10.1016/j.oraloncology.2011.11.012
Loprinzi, C.E., Prasad, K., Schroeder, D.R., & Sood, A. (2011). Stress Management and Resilience Training (SMART) program to decrease stress and enhance resilience among breast cancer survivors: A pilot randomized clinical trial. Clinical Breast Cancer, 11(6), 364–368. https://doi.org/10.1016/j.clbc.2011.06.008
MacKillop, J., & Anderson, E.J. (2007). Further psychometric validation of the Mindful Attention Awareness Scale (MAAS). Journal of Psychopathology and Behavioral Assesment, 29(4), 289–293. https://doi.org//10.1007/s10862-007-9045-1
Magtibay, D.L., Chesak, S.S., Coughlin, K., & Sood, A. (2017). Decreasing stress and burnout in nurses: Efficacy of blended learning with stress management and resilience training program. Journal of Nursing Administration, 47(7–8), 391–395. https://doi.org/10.1097/NNA.0000000000000501
Melin-Johansson, C., Henoch, I., Strang, S., & Browall, M. (2012). Living in the presence of death: An integrative literature review of relatives’ important existential concerns when caring for a severely ill family member. Open Nursing Journal, 6, 1–12. https://doi.org/10.2174/1874434601206010001
Milbury, K., Li, Y., Durrani, S., Liao, Z., Tsao, A.S., Carmack, C., . . . Bruera, E. (2020). A mindfulness-based intervention as a supportive care strategy for patients with metastatic non–small cell lung cancer and their spouses: Results of a three-arm pilot randomized controlled trial. Oncologist, 25(11), e1794–e1802. https://doi.org/10.1634/theoncologist.2020-0125
Morris, N.S., & Rosenbloom, D.A. (2017). Defining and understanding pilot and other feasibility studies. American Journal of Nursing, 117(3), 38–45. https://doi.org/10.1097/01.NAJ.0000513261.75366.37
National Alliance for Caregiving. (2016). Cancer caregiving in the U.S. An intense, episodic, and challenging care experience. https://www.caregiving.org/wp-content/uploads/2020/05/CancerCaregivingR…
National Alliance for Caregiving. (2021). Caregiving in a diverse America: Beginning to understand the systemic challenges facing family caregivers. https://www.caregiving.org/wp-content/uploads/2021/12/NAC_AmgenDiverseC…
National Cancer Institute. (2022). Informal caregivers in cancer: Roles, burden, and support (PDQ®)—Health professional version. https://www.cancer.gov/about-cancer/coping/family-friends/family-caregi…
Neff, K.D., & Dahm, K.A. (2015). Self-compassion: What it is, what it does, and how it relates to mindfulness. In B.D. Ostafin, M.D. Robinson, & B.P. Meier (Eds.), Handbook of mindfulness and self-regulation (pp. 121–137). Springer.
Neff, K.D., & Pommier, E. (2013). The relationship between self-compassion and other-focused concern among college undergraduates, community adults, and practicing meditators. Self and Identity, 12(2), 160–176.
Northouse, L.L., Katapodi, M.C., Schafenacker, A.M., & Weiss, D. (2012). The impact of caregiving on the psychological well-being of family caregivers and cancer patients. Seminars in Oncology Nursing, 28(4), 236–245. https://doi.org/10.1016/j.soncn.2012.09.006
Northouse, L.L., Williams, A.-L., Given, B., & McCorkle, R. (2012). Psychosocial care for family caregivers of patients with cancer. Journal of Clinical Oncology, 30(11), 1227–1234. https://doi.org/10.1200/jco.2011.39.5798
Paek, M.-S., Nightingale, C.L., Tooze, J.A., Milliron, B.-J., Weaver, K.E., & Sterba, K.R. (2018). Contextual and stress process factors associated with head and neck cancer caregivers’ physical and psychological well-being. European Journal of Cancer Care, 27(2), e12833. https://doi.org/10.1111/ecc.12833
Peterson, A.L., Blount, T.H., & McGeary, D.D. (2014). Stress and psychological resiliency. In C. Pariante, M. Lapiz-Bluhm (Eds.). Behavioral neurobiology of stress-related disorders. (pp. 297–312). Current Topics in Behavioral Neurosciences, 18. Springer. https://doi.org/10.1007/7854_2014_293
Raes, F., Pommier, E., Neff, K.D., & Van Gucht, D. (2011). Construction and factorial validation of a short form of the Self-Compassion Scale. Clinical Psychology and Psychotherapy, 18(3), 250–255. https://doi.org/10.1002/cpp.702
Resilient Option. (n.d.). Online program. https://www.resilientoption.com/online-program
Schellekens, M.P.J., Karremans, J.C., van der Drift, M.A., Molema, J., van den Hurk, D.G.M., Prins, J.B., & Speckens, A.E.M. (2017). Are mindfulness and self-compassion related to psychological distress and communication in couples facing lung cancer? A dyadic approach. Mindfulness, 8(2), 325–336. https://doi.org/10.1007/s12671-016-0602-0
Schlichting, J.A., Pagedar, N.A., Chioreso, C., Lynch, C.F., & Charlton, M.E. (2019). Treatment trends in head and neck cancer: Surveillance, Epidemiology, and End Results (SEER) patterns of care analysis. Cancer Causes and Control, 30(7), 721–732. https://doi.org/10.1007/s10552-019-01185-z
Shapiro, S.L., Carlson, L.E., Astin, J.A., & Freedman, B. (2006). Mechanisms of mindfulness. Journal of Clinical Psychology, 62(3), 373–386. https://doi.org/10.1002/jclp.20237
Shin, K.J., Lee, Y.J., Yang, Y.R., Park, S., Suh, P.-G., Follo, M.Y., . . . Ryu, S.H. (2016). Molecular mechanisms underlying psychological stress and cancer. Current Pharmaceutical Design, 22(16), 2389–2402. https://doi.org/10.2174/1381612822666160226144025
Simpson, G.K., Dall’Armi, L., Roydhouse, J.K., Forstner, D., Daher, M., Simpson, T., & White, K.J. (2015). Does resilience mediate carer distress after head and neck cancer? Cancer Nursing, 38(6), E30–E36.
Sinclair, S., McClement, S., Raffin-Bouchal, S., Hack, T.F., Hagen, N.A., McConnell, S., & Chochinov, H.M. (2016). Compassion in health care: An empirical model. Journal of Pain and Symptom Management, 51(2), 193–203. https://doi.org/10.1016/j.jpainsymman.2015.10.009
Song, L., Qan’ir, Y., Guan, T., Guo, P., Xu, S., Jung, A., . . . Kent, E.E. (2021). The challenges of enrollment and retention: A systematic review of psychosocial behavioral interventions for patients with cancer and their family caregivers. Journal of Pain and Symptom Management, 62(3), e279–e304. https://doi.org/10.1016/j.jpainsymman.2021.04.019
Sood, A. (2013). The Mayo Clinic guide to stress-free living. Da Capo Lifelong Books.
Sood, A., & Jones, D.T. (2013). On mind wandering, attention, brain networks, and meditation. Explore, 9(3), 136–141. https://doi.org/10.1016/j.explore.2013.02.005
Sood, A., Prasad, K., Schroeder, D., & Varkey, P. (2011). Stress management and resilience training among department of medicine faculty: A pilot randomized clinical trial. Journal of General Internal Medicine, 26(8), 858–861. https://doi.org/10.1007/s11606-011-1640-x
Sood, A., Sharma, V., Schroeder, D.R., & Gorman, B. (2014). Stress Management and Resiliency Training (SMART) program among department of radiology faculty: A pilot randomized clinical trial. Explore, 10(6), 358–363. https://doi.org/10.1016/j.explore.2014.08.002
Stonnington, C.M., Darby, B., Santucci, A., Mulligan, P., Pathuis, P., Cuc, A., . . . Sood, A. (2016). A resilience intervention involving mindfulness training for transplant patients and their caregivers. Clinical Transplantation, 30(11), 1466–1472. https://doi.org/10.1111/ctr.12841
Williams, A.-L., & McCorkle, R. (2011). Cancer family caregivers during the palliative, hospice, and bereavement phases: A review of the descriptive psychosocial literature. Palliative and Supportive Care, 9(3), 315–325. https://doi.org/10.1017/s147895151100026


